Eye Treatments
Eye Injections
Intraocular injections, or Anti-VEGF medicines, improve vision in every third patient treated and stabilise vision in at least nine out of ten cases.
Currently, wet macular degeneration is mainly treated with the following medications:
- Bevacizumab (Avastin)
- Beovu® (Brolucizumab); its active substance, brolucizumab, is an anti-neovascularisation medication. Beovu is used to treat neovascular (wet) age-related degeneration in adults. It is injected into the eye by a doctor.
- Aflibercept (Eylea)
- Ranibizumab (Lucentis)
- Avastin is on the list of pharmaceuticals reimbursed by the Estonian Health Insurance Fund.
Referenced: https://www.aao.org/eye-health/drugs/anti-vegf-treatments

A blue line leads from the reception to the injection department.

Injection procedure office assistant Heli Rumm and Dr. Aleksei Detotšenko prepare for the next patient.
Purpose
Intraocular injections are used to treat a number of eye conditions, such as age-related macular degeneration (wet form), diabetes-induced retinal edema or vitreous hemorrhage, retinal edema due to blood vessel closure in the ocular fundus, neovascular glaucoma, and retinal edema due to other eye diseases. Patients often need these injections repeatedly.

Optometrist Regina Entson conducting a Spectralis scan.
Procedure
The medicine is delivered into the vitreous inside the eye via an intraocular injection. This route of administration helps to increase the concentration of the medication in the eye and to avoid the side effects that may occur with systemic administration.
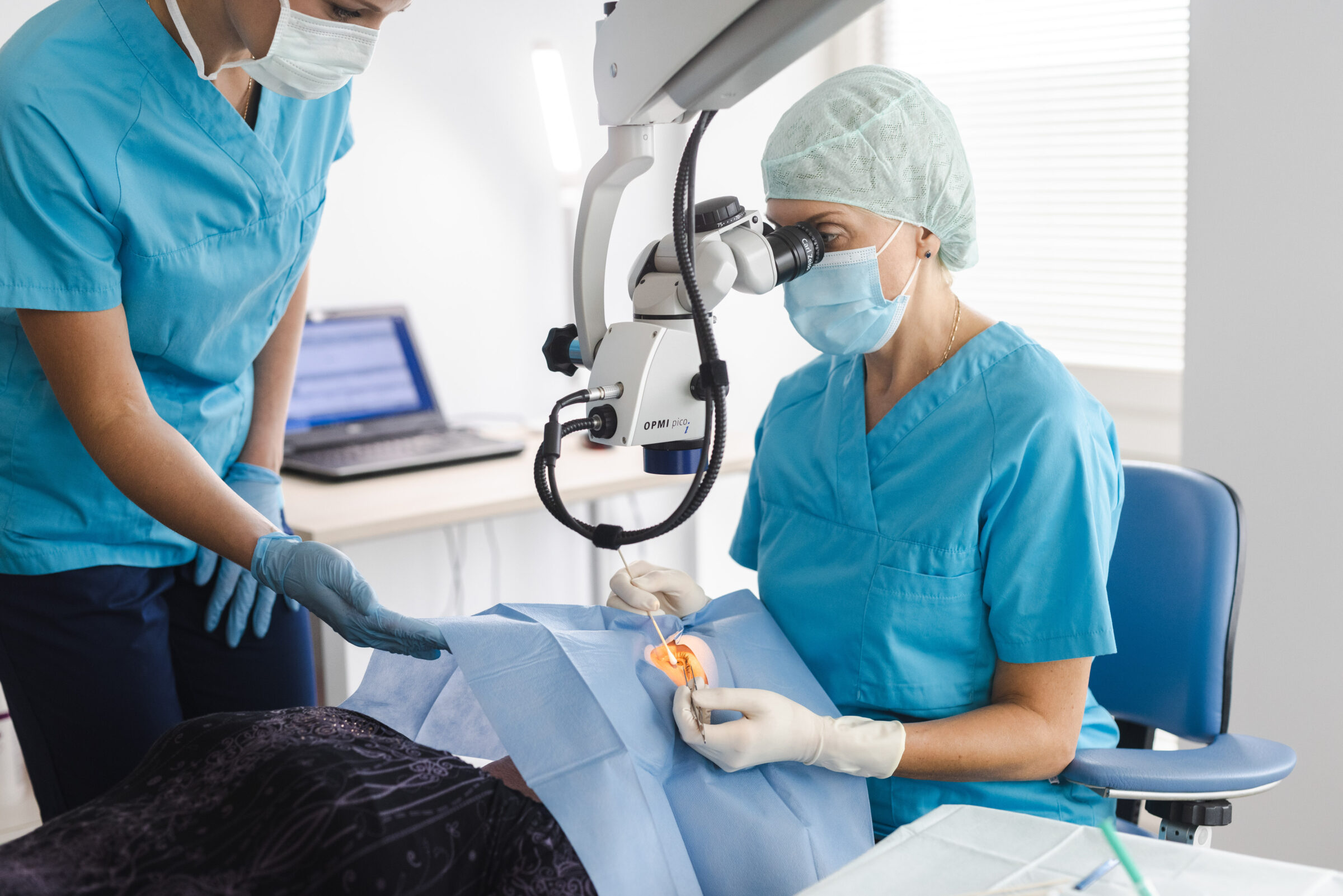
Dr. Margarita Rebrov and injection nurse Anna Jaroslavtseva performing the procedure.
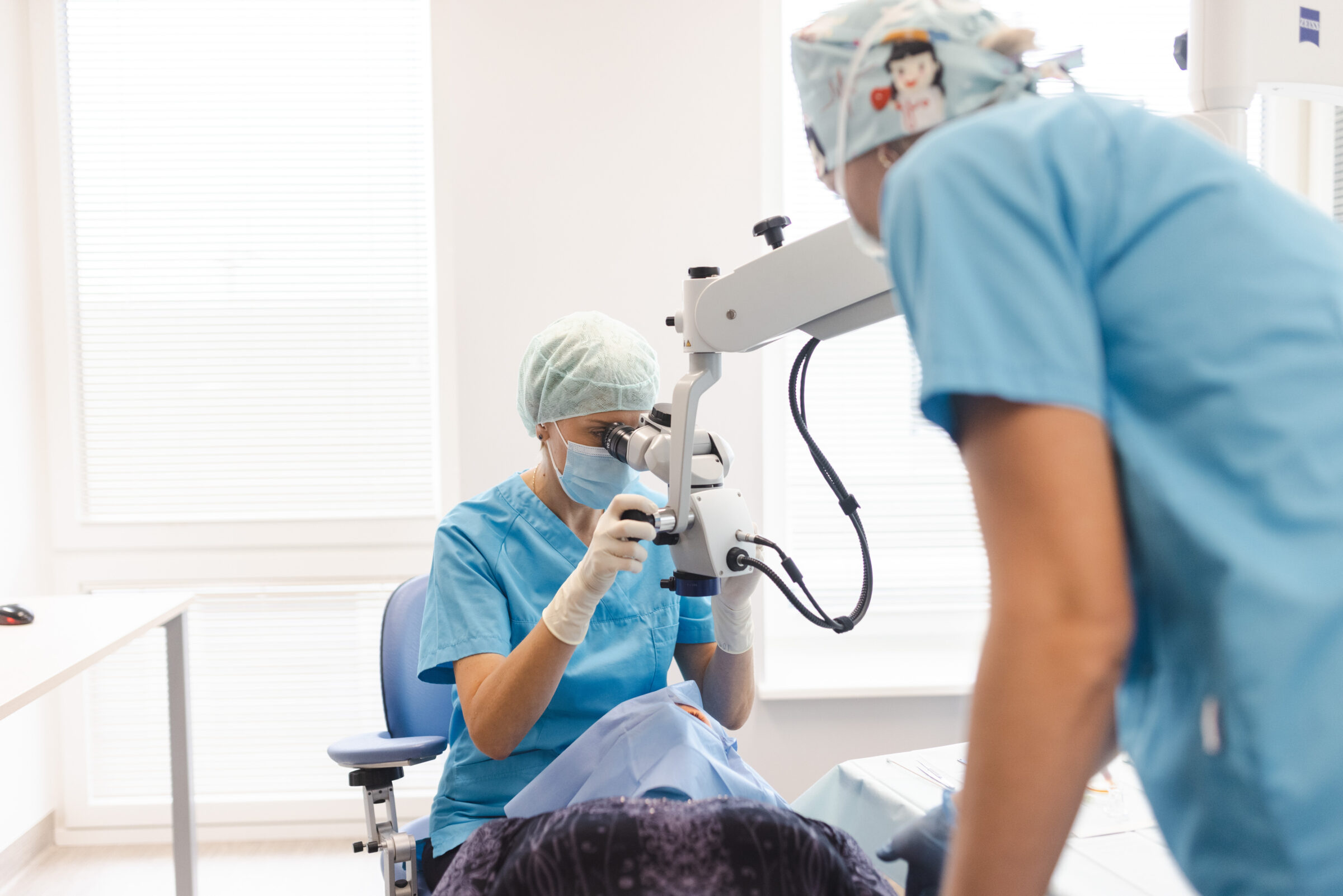
Patients often need the aid of Dr. Margarita Rebrovi and injection nurse Anna Jaroslavtseva repeatedly.
How long does the procedure take?
Please allow up to two hours for the procedure and related examinations. As the patients’ waiting room has limited space, we ask the company of the visitor to not wait for the patient inside the clinic during the appointment.
How to prepare for the procedure?
- No change in your usual lifestyle or medication (including eye drops) is needed before the intraocular injection. Do not use make-up on the day of the injection.
- In the case of an eye infection, an infection of the upper respiratory tract, or other acute illness, the injection appointment must be postponed and rescheduled.
- Prior to the injection, you will be asked to sign a consent form regarding the procedure.
- The nurse will measure your intraocular pressure before the injection, perform refractometry and other tests if necessary.
- Pupil-dilating eye drops are instilled into the eye, resulting in blurry vision for several hours.
- Before the injection, anesthetic eye drops will be instilled. You will receive plastic slippers and a hat to put on. Furthermore, an additional eye examination will be performed by the doctor. If the eye is inflamed, for example, a respective treatment will be designated and the injection appointment rescheduled.
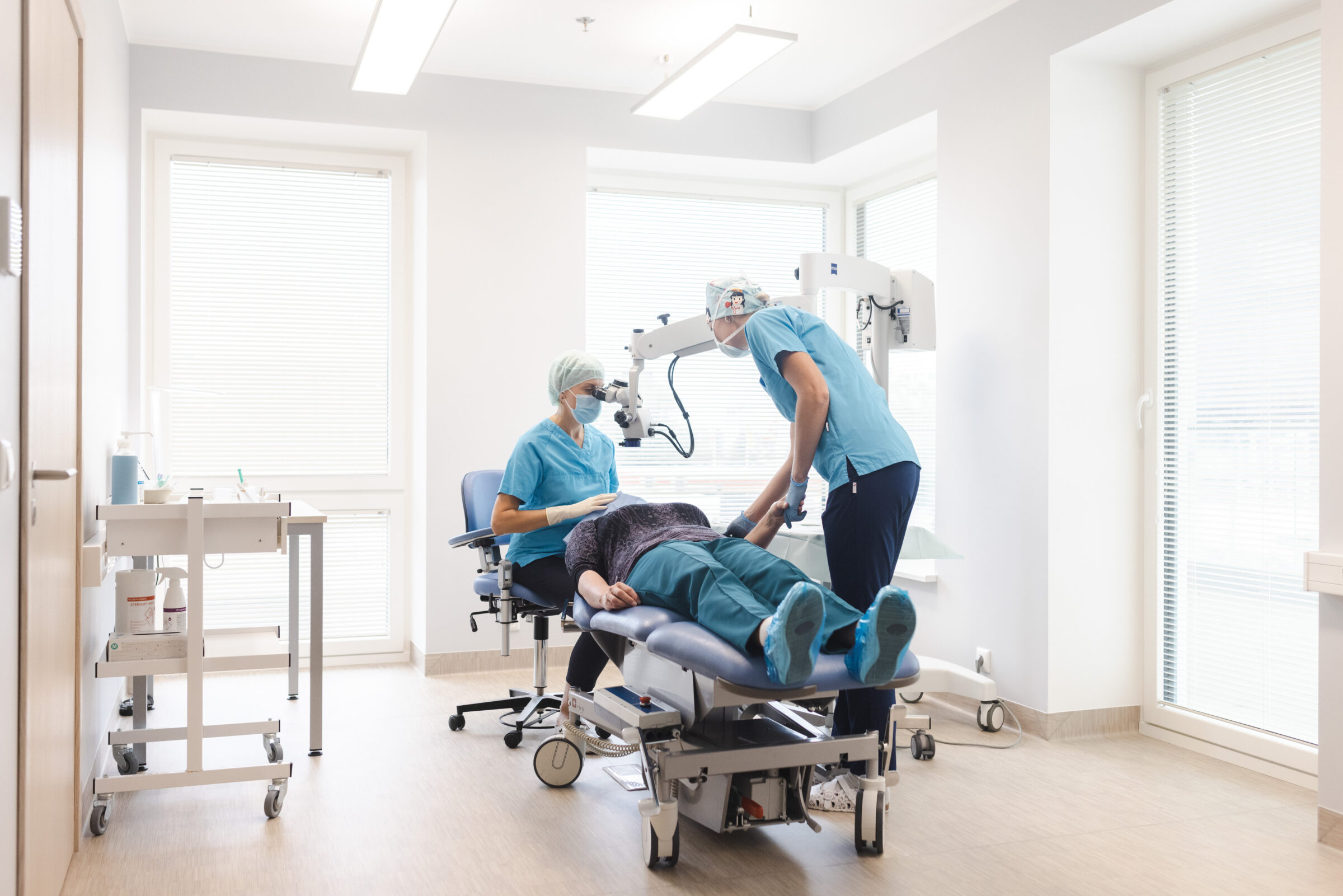
The whole procedure takes less than 10 minutes.
What to expect during the procedure?
- The injection is performed in a lying position under sterile conditions in the procedure room.
- First, the eye and its surrounding area are cleansed with dilute iodine solution. A sterile sheet is then placed on the face, leaving only the eye to be injected exposed. Talking in the procedure room should be avoided to ensure sterility.
- The injection is performed using a very fine needle and directed through the part of the eye without blood vessels or a risk of retinal damage. Injecting the medicine into the vitreous is typically rather painless. The whole procedure takes less than 10 minutes.
- A sterile bandage is placed over the eye after the injection. You will be asked to sit in the waiting room for a while. The nurse will then remove the bandage and check the intraocular pressure. You are then discharged from the clinic.
What to consider after the procedure?
- Do not rub or otherwise touch the eye after the injection, as anesthetic eye drops will continue to work for some time and there is a risk of injury to the eye surface.
- Do not drive immediately after the injection, as your visual acuity may be reduced as a result of the pupil-dilating eye drops.
- After the injection, you may experience tingling, and the sensation of debris in the eye. There might be a slight redness in the eye. These occurences will pass in a few days. The use of moisturizing eye drops will help relieve these symptoms (a new bottle is recommended after each injection).
- Sometimes, a bruise may develop under the mucous membrane at the injection site – a red spot or a larger red patch. It is not harmful to the vision and will resolve without treatment in 10 to 14 days.
- After the injection, dark floating spots may occur in front of the eye due to the medication or tiny air bubbles. They decrease and disappear gradually and do not impose any danger to the vision.
- You will also be scheduled for a check-up appointment with your doctor after your visit. If necessary, a follow-up injection appointment will be arranged.
- If you have been prescribed other medicines, including eye drops (e.g. for glaucoma treatment), continue with your usual schedule after the injection.
- Do not go swimming, bathing, nor should you visit a swimming pool or a sauna for two days post-injection. When taking a shower, avoid getting water in your eyes.
- Rarely (less than 1 in 1,000 injections), serious vision impairing complications, such as endophthalmitis (intraocular inflammation), retinal tears, eye lens damage, intraocular hemorrhage, and closure of the central artery of the eye, have occurred after an intraocular injection.
When to see a doctor immediately?
If you experience severe pain, your eye becomes intensely red (or cloudy) or your vision deteriorates significantly after the injection, you should contact your ophthalmologist immediately (tel. 655 6244) or contact an ophthalmologist at the East Tallinn Central Hospital (Ravi tn 18, Tallinn) during non-working hours. These symptoms may indicate serious post-injection complications.





